Competing priorities have kept me away from this site in recent weeks. There’s been work to do on COCAPP, which is close to the finish line, and doctoral students’ drafts to read and comment on (before imminent thesis submission, in one case). I’ve also been reading a thesis ahead of a PhD examination I’m involved in at the end of the coming week. So if this catch-up post feels a little bitty, then that’s because it is: there’s been lots happening that I want to comment on.
First up is the RiSC study, which I’ve mentioned here plenty of times before. In the last ten or so days the NIHR has published a first look summary of our aims, methods and findings. This is a precursor to the publication of our whole report, which is now post-peer review. Sometime in the new year we’ll be reconvening as a research team to plan our next project.
In October I made the short trip to the University of South Wales to hear Professor Linda Aiken from the University of Pennsylvania deliver this year’s RCN Winifred Raphael Lecture. Professor Aiken spoke on Quality nursing care: what makes a difference?, drawing on findings from the RN4Cast study and more. As promised, the RCN Research Society has now uploaded its video of the event for the world to see. It’s well worth watching.
News on the Mental Health Nurse Academics UK front includes an election, which we are now midway through, for the group’s next Vice Chair and Chair Elect. I’m overseeing this process (as I’ve done twice before), and will be in a position to announce the successful nominee on December 15th. One of the things that MHNAUK does is to work with the RCN to run the annual NPNR conference, and I’m very pleased to have had the chance to join the NPNR scientific and organising committee for a three year stint. More to follow on that front in the future, including details of next year’s event as they emerge.
Elsewhere I read that the Shape of Caring review, chaired by Lord Willis, is looking at the UK practice of preparing new nurses, at the point of registration, for work in one of four fields (mental health, adult, child and learning disability). This is something to keep a close eye on, with reports from last month’s Chief Nursing Officer Summit in England suggesting that the fields may be on their way out. For a useful, balanced, review in this area I refer the reader to the 2008 King’s College London Policy+ paper Educating students for mental health nursing practice: has the UK got it right? and, for a longer read, to Approaches to specialist training at pre-registration level: an international comparison.
Follow @benhannigan Here’s a post to draw attention to the
Here’s a post to draw attention to the 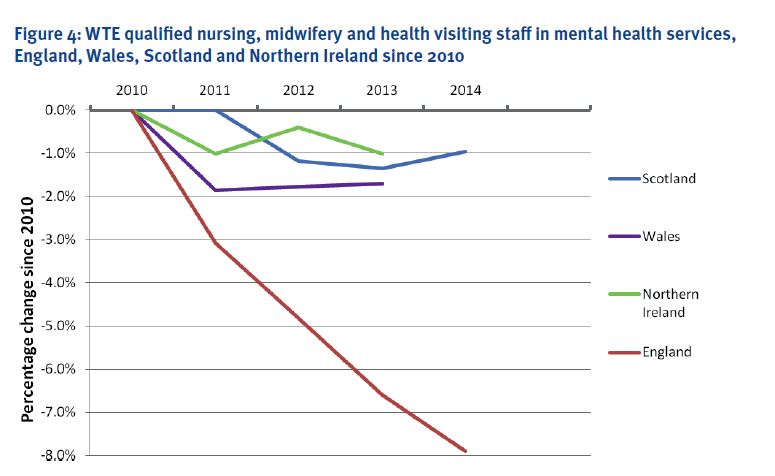
 I’m just back from Horatio’s latest gathering: the
I’m just back from Horatio’s latest gathering: the 
 For those not at the 20th International Network for Psychiatric Research Conference, which took place yesterday and the day before at Warwick University, here are links to the
For those not at the 20th International Network for Psychiatric Research Conference, which took place yesterday and the day before at Warwick University, here are links to the 